Flexible sigmoidoscopy
What is a flexible sigmoidoscopy?
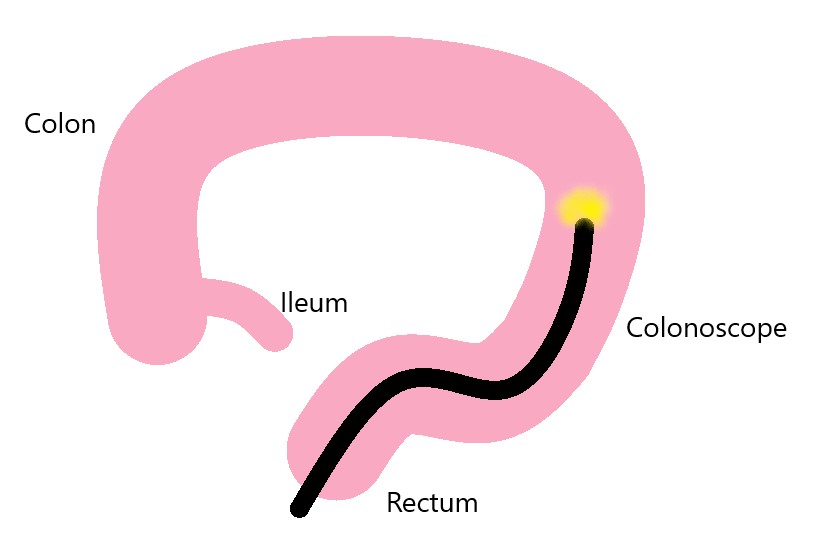
A flexible sigmoidoscopy is similar to a colonoscopy except that only the rectum and lower colon (sigmoid or descending colon) is examined. It is usually performed only for specific reasons, e.g. surveillance of inflammatory bowel disease or assessment of rectal bleeding, using a colonoscope.
During the examination, a number of small procedures can also be carried out, including:
Taking a small tissue sample (biopsy)
Removal of polyps – a growth on the surface layer of colon or rectum. Some polyps may become bowel cancer and can be removed by your gastroenterologist when detected
Risks of a flexible sigmoidoscopy
Complications are rare, but can occur and include bleeding or perforation. If you notice symptoms of severe abdominal pain, abdominal distention, unexplained fevers or significant rectal bleeding (e.g. more than half a cup) up to 2 weeks after your procedure, please inform your gastroenterologist or present to the emergency department for assessment.
Preparation
You will be advised to fast for at least 6 hours before your procedure. The rectum and lower colon must be cleared of stool to allow a successful procedure. This is done by administering one or two enemas prior to your procedure. Most medications can be continued before the flexible sigmoidoscopy, but please inform your gastroenterologist if you are on any blood thinning medications as these may need to be withhold.
What happens during a flexible sigmoidoscopy?
You will lie on your left side and intravenous sedation is usually administered. Some patients may elect to have their procedure without sedation as the procedure is well tolerated and rarely causes discomfort. The intestinal lining is carefully examined and may be biopsied or have polyps removed depending on the findings. Gas and water is injected to distend the bowel to allow adequate examination; sometimes this may cause a feeling or bloating or cramping.
After a flexible sigmoidoscopy
Any sensations of bloating or abdominal cramping should quickly improve with passage of gas following your procedure. You should be able to eat soon after the procedure. If you received sedation, you must not drive or sign important documents for 24 hours. Your gastroenterologist will advise whether any follow-up with themselves or with your GP is required to discuss results of the procedure or biopsy specimens taken.
If you require help
Please:
Call our practice during working hours (9am – 5pm, Monday to Friday)
- Speak with your GP
- Call Health Direct
- Attend your nearest emergency department or call 000
